The ability to move freely and without pain is often taken for granted until the subtle onset of stiffness or discomfort begins to limit daily activities. Joint health is the cornerstone of physical independence, serving as the literal pivot point for every action from walking to fine motor tasks. By understanding the biological mechanisms of our musculoskeletal system, we can implement proactive strategies to preserve cartilage and prevent the onset of degenerative conditions. Prioritizing joint integrity today is the most effective way to ensure a mobile, active, and pain-free future.
Understanding Joint Health Prevent Arthritis Mobility: What Science Says
According to the World Health Organization (WHO) in 2023, musculoskeletal conditions are the leading contributor to disability worldwide, affecting approximately 1.71 billion people globally. These conditions significantly limit mobility and dexterity, leading to early retirement from the workforce and lower levels of well-being. Arthritis is not a single disease but an informal way of referring to joint pain or joint disease, with over 100 different types identified by medical science. The most common form, osteoarthritis, involves the wear and tear of the protective cartilage that cushions the ends of the bones.
Recent data from the Centers for Disease Control and Prevention (CDC) in 2023 indicates that roughly 58.5 million adults in the United States have doctor-diagnosed arthritis, a number expected to rise as the population ages. The science of joint health emphasizes that while aging is a factor, it is not the sole cause of joint degradation. Factors such as systemic inflammation, mechanical stress, and metabolic health play critical roles in how our joints hold up over time. By addressing these factors through lifestyle interventions, individuals can significantly reduce their risk of developing chronic joint issues and maintain high levels of mobility well into their later years.
The Biological Mechanics of Joint Longevity

📷 Image via kabe32 on Pixabay
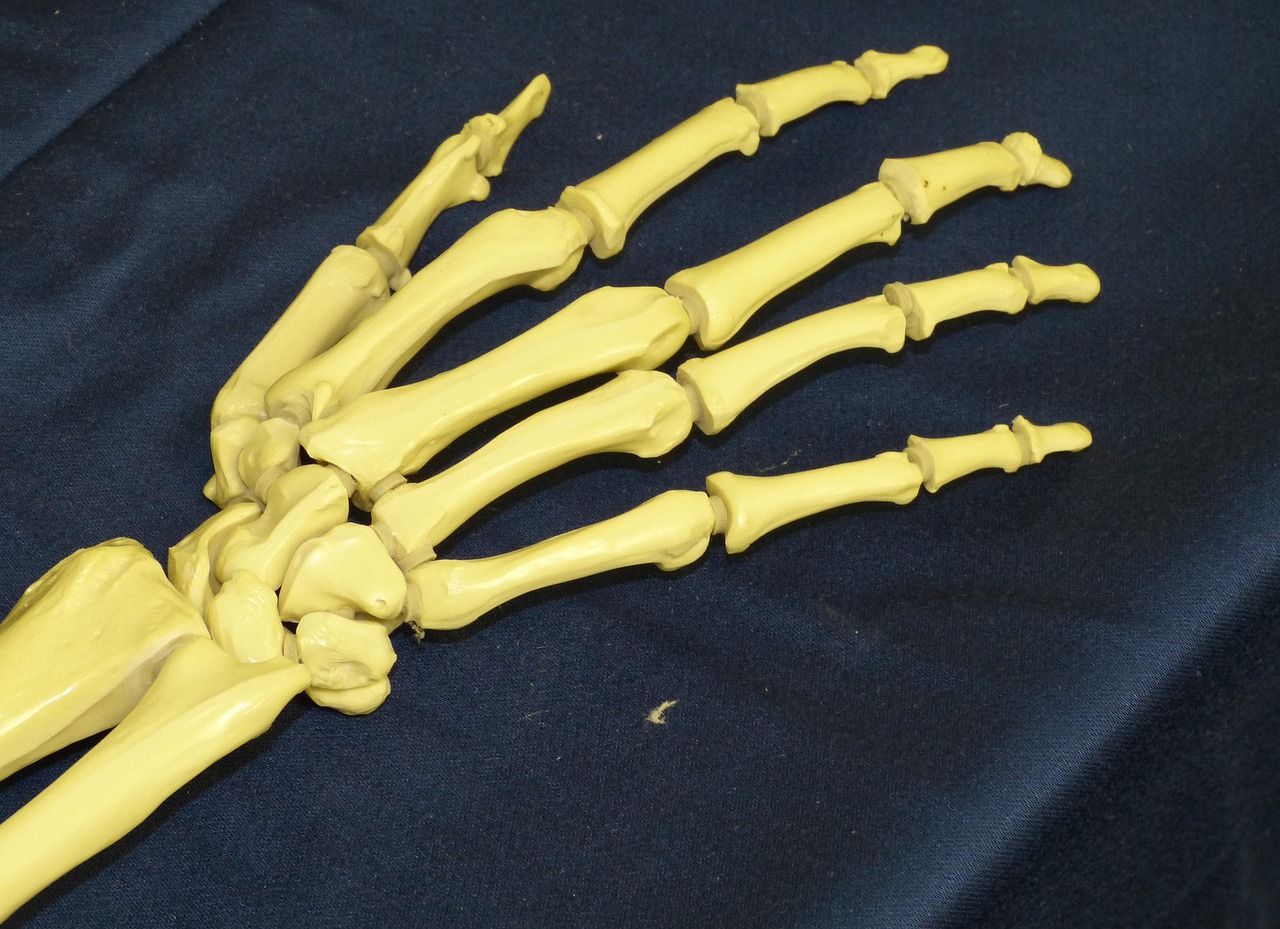
To prevent arthritis, one must first understand the anatomy of a healthy joint. A joint is the meeting point of two or more bones, held together by ligaments and cushioned by a layer of articular cartilage. This cartilage is a firm, slippery tissue that allows for near-frictionless motion. Surrounding the joint is the synovium, a membrane that produces synovial fluid. This fluid acts as both a lubricant and a shock absorber, while also delivering essential nutrients to the cartilage, which lacks its own blood supply. When this system is compromised—either through injury, lack of nutrients, or excessive pressure—the cartilage begins to thin, leading to the bone-on-bone contact characteristic of arthritis.
Maintaining the health of the synovium and the quality of the synovial fluid is vital for long-term mobility. Movement itself is the primary mechanism for “feeding” the joints; because cartilage is porous, the compression and release during physical activity pump nutrients into the tissue and flush out metabolic waste. This is why sedentary lifestyles are often linked to stiffer joints and accelerated degeneration. Furthermore, the strength of the surrounding musculature provides a secondary support system, absorbing the impact of movement before it reaches the delicate joint structures. A holistic approach to joint health must therefore focus on both the internal environment of the joint and the external support provided by muscles and tendons.
Weight Management as a Primary Preventive Pillar
One of the most significant factors in preventing arthritis and preserving mobility is maintaining a healthy body weight. The relationship between weight and joint health is purely mechanical: for every pound of body weight gained, there is a four-pound increase in pressure on the knees and a six-fold increase in pressure on the hips during daily activities like walking. Over time, this compounded stress accelerates the breakdown of articular cartilage, making obesity one of the most significant modifiable risk factors for osteoarthritis. The CDC (2023) notes that adults with obesity are much more likely to be diagnosed with arthritis than those at a healthy weight.
Beyond the mechanical stress, adipose tissue (body fat) is metabolically active and produces pro-inflammatory cytokines. These chemicals circulate through the bloodstream and can cause systemic inflammation that specifically targets joint tissues. This explains why individuals with high body fat percentages often experience arthritis in non-weight-bearing joints, such as those in the hands. By achieving and maintaining a healthy weight, individuals can simultaneously reduce the physical load on their joints and lower the chemical triggers of inflammation, creating a dual-layered defense against degenerative joint disease.
Anti-Inflammatory Nutrition for Joint Integrity
Diet plays a transformative role in joint health by either fueling or quenching the fires of inflammation. An anti-inflammatory diet, often modeled after the Mediterranean style of eating, is rich in omega-3 fatty acids, antioxidants, and phytochemicals that protect joint tissues. Omega-3 fatty acids, found in fatty fish like salmon, walnuts, and flaxseeds, are particularly effective at reducing the production of enzymes that break down cartilage. Studies have shown that consistent intake of these healthy fats can reduce joint morning stiffness and the number of painful joints in people with early-stage inflammatory conditions.
In addition to healthy fats, the consumption of colorful fruits and vegetables provides the body with the antioxidants necessary to combat oxidative stress in the joints. For example, anthocyanins found in cherries and berries have been linked to lower levels of C-reactive protein, a marker of systemic inflammation. Cruciferous vegetables like broccoli contain sulforaphane, a compound that may block enzymes that cause joint destruction. Furthermore, incorporating spices like turmeric and ginger can provide natural anti-inflammatory benefits. Turmeric contains curcumin, which has been shown in various clinical trials to rival the efficacy of some over-the-counter pain relievers in managing joint discomfort without the gastrointestinal side effects.
The Role of Low-Impact Exercise in Mobility

📷 Image via 7854 on Pixabay
While it may seem counterintuitive to move joints that feel stiff or vulnerable, exercise is essential for preventing the progression of arthritis. The key lies in selecting low-impact activities that strengthen the body without placing undue stress on the joints. Swimming and water aerobics are often considered the “gold standard” for joint-friendly exercise because the buoyancy of water supports the body’s weight, allowing for a full range of motion with minimal impact. Cycling is another excellent option, as it builds leg strength—specifically the quadriceps—which helps stabilize the knee joint and protect it from jarring forces during walking.
Strength training is equally important for joint health. When the muscles surrounding a joint are strong, they act as a “shock absorber,” taking the brunt of the force from daily movements. For instance, strong gluteal and core muscles help maintain proper pelvic alignment, which reduces the risk of hip and lower back issues. It is important to focus on functional movements and proper form rather than lifting maximum weights. Incorporating flexibility and balance exercises, such as yoga or Tai Chi, can also improve proprioception—the body’s ability to sense its position in space—which reduces the risk of falls and acute joint injuries that could lead to post-traumatic arthritis later in life.
Ergonomics and Joint Protection in Daily Life
Modern lifestyles often involve repetitive motions or prolonged static postures that can wreak havoc on joint health over decades. Ergonomics—the science of fitting the workplace to the user—is a critical component of arthritis prevention. For those who work at a desk, ensuring that the computer screen is at eye level, the chair provides adequate lumbar support, and the feet are flat on the floor can prevent chronic strain on the neck, shoulders, and lower back. Small adjustments, such as using a vertical mouse or an ergonomic keyboard, can also prevent the development of repetitive strain injuries in the wrists and fingers.
Beyond the office, joint protection involves being mindful of how we use our bodies during everyday chores. For example, when lifting heavy objects, one should always bend at the knees and hips rather than the waist, using the powerful muscles of the legs to do the work. Carrying groceries or bags using the palms of the hands or the forearms rather than just the fingers can distribute the load and protect the small joints of the hand. Recognizing the early signs of joint fatigue and allowing for rest and recovery is also essential. Pushing through sharp pain can lead to micro-tears in the ligaments or tendons, which eventually compromises the stability of the entire joint complex.
Hydration and the Role of Synovial Fluid
Hydration is a frequently overlooked aspect of joint health. As previously mentioned, cartilage is composed of approximately 70% to 80% water. When the body is dehydrated, it may pull water from the joints to support more critical functions like brain and heart health. This reduction in water content makes the cartilage less resilient and more prone to damage. Furthermore, the synovial fluid that lubricates the joints requires adequate hydration to maintain its viscosity. Without enough water, this fluid becomes thinner and less effective at preventing friction between the bones.
To support joint lubrication, it is recommended to maintain consistent water intake throughout the day rather than consuming large amounts all at once. While individual needs vary, the general guideline of eight glasses a day is a good starting point, with adjustments made for activity level and climate. In addition to plain water, consuming hydrating foods like cucumbers, watermelon, and celery can contribute to the body’s total fluid balance. Avoiding excessive caffeine and alcohol, which can have diuretic effects, also helps ensure that the joints remain properly lubricated and cushioned against the stresses of movement.
Early Detection and Professional Intervention
Preventing arthritis and maintaining mobility requires a proactive approach to medical care. Many people wait until joint pain is debilitating before seeking professional advice, but early intervention can often halt or significantly slow the progression of joint damage. If you experience joint swelling, redness, or stiffness that lasts for more than two weeks, a consultation with a healthcare provider or a rheumatologist is warranted. Diagnostic tools such as X-rays, MRIs, and blood tests can help identify the specific type of joint issue and allow for a targeted treatment plan.
Professional intervention may also include physical therapy, which is one of the most effective non-surgical treatments for joint health. A physical therapist can identify muscle imbalances, gait abnormalities, and postural issues that are contributing to joint strain. They can provide a customized exercise program designed to strengthen specific support muscles and improve joint range of motion. In some cases, supplements such as glucosamine and chondroitin may be recommended, although their efficacy varies by individual. By combining medical expertise with the lifestyle strategies discussed, individuals can create a comprehensive “joint-protection plan” that ensures mobility and independence for a lifetime.

