In This Article
- How Functional Mobility Exercises Support Joint Stability and Movement Efficiency
- Common Daily Movements That Mask Hidden Instability
- Evidence-Based Strategies to Restore Safe Movement Patterns
- Cutting-Edge Research and Clinical Recommendations
- Frequently Asked Questions
- Conclusion and Key Takeaways
Every time you bend to lift a grocery bag or twist to check your blind spot, your body performs a complex choreography of muscle contractions, joint rotations, and neurological signals. When this system works seamlessly, these movements feel effortless. But when muscular imbalances or joint restrictions develop, daily tasks become gateways to pain, stiffness, or even serious injury.
- Optimizing Sleep for Peak Athletic Recovery and Performance Boost
- Resistance Training Safeguards Bone Health and Prevents Osteoporosis with Age
- Functional Mobility Exercises Reduce Daily Injury Risk Through Muscle Balance
- Progressive Weightlifting Slows Osteoporosis and Strengthens Aging Bones
- HIIT Outperforms Steady Cardio for Heart Health Benefits
Statistics from the World Health Organization show that musculoskeletal conditions affect 1.7 billion people globally, making them the leading contributor to years lived with disability worldwide. In the United States alone, the Centers for Disease Control and Prevention reports that 25% of adults experience low back pain each year, with similar trends reported across Europe and Asia. While aging contributes to joint degeneration, research increasingly points to preventable movement dysfunctions as a primary driver of these statistics. Functional mobility exercises-corrective movements designed to restore natural joint mechanics and muscular balance-have emerged as a powerful, evidence-based strategy to reduce injury risk during everyday activities.

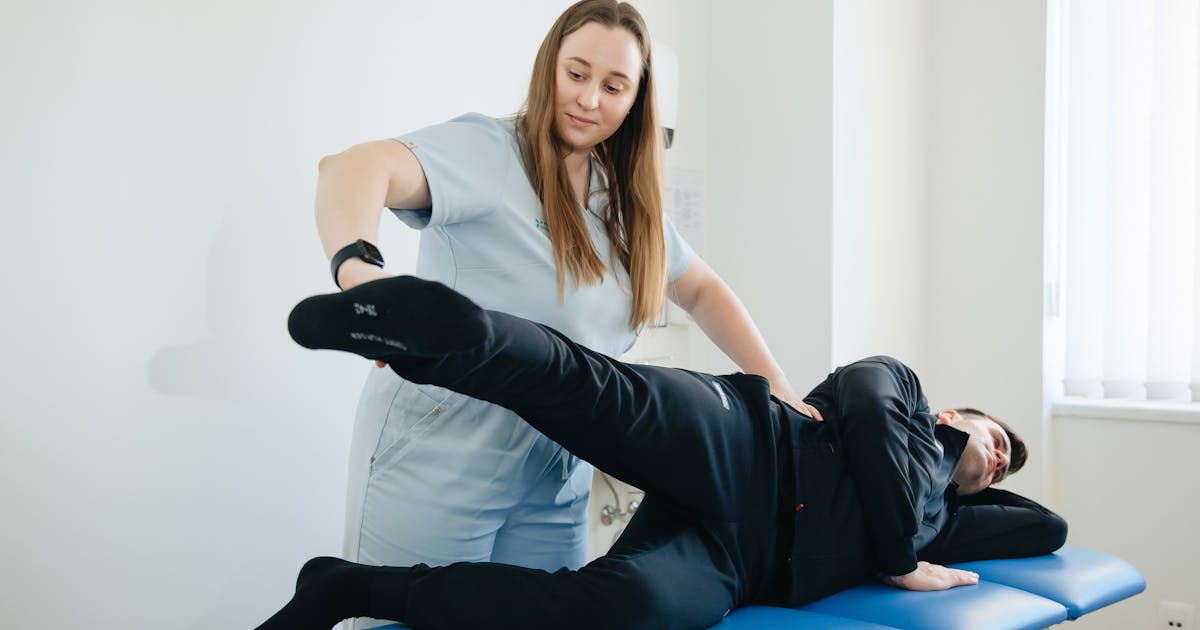
Photo by Funkcinės Terapijos Centras on Pexels
How Functional Mobility Exercises Support Joint Stability and Movement Efficiency
At the core of functional mobility lies the principle of arthrokinematic motion-the subtle gliding and rolling of joint surfaces that enables smooth movement. When joints lose their optimal alignment due to prolonged sitting, repetitive motions, or previous injuries, surrounding muscles compensate by over-activating certain groups while others become inhibited. This imbalance shifts load distribution, placing excessive strain on ligaments, tendons, and cartilage-ultimately increasing injury risk during basic movements like squatting, reaching overhead, or walking.
Neuromuscular control-the brain’s ability to coordinate muscle activation with joint position-deteriorates when movement patterns become inefficient. A 2022 study in the *Journal of Athletic Training* found that individuals with chronic low back pain exhibited delayed activation of the transverse abdominis muscle during lifting tasks, a delay associated with a 3.4-fold higher risk of reinjury. Functional mobility training targets this deficit by engaging stabilizer muscles through controlled, multiplanar movements, effectively “re-wiring” the nervous system for safer, more coordinated motion.
Beyond neuromuscular efficiency, functional mobility exercises enhance tissue resilience by improving joint capsule mobility and fascial extensibility. The hip joint, for example, relies on a balance of mobility between flexion-extension, abduction-adduction, and internal-external rotation. When hip flexors tighten (common in desk workers), posterior pelvic tilt and compensatory lumbar flexion occur during squatting, increasing shear forces on lumbar discs. Targeted mobility drills-such as controlled hip CARs (controlled articular rotations)-have been shown in a 2023 systematic review in *Sports Medicine* to improve hip internal rotation range of motion by an average of 12 degrees within six weeks, significantly reducing compensatory lumbar movement during daily tasks.
Common Daily Movements That Mask Hidden Instability
Certain seemingly harmless activities are frequent culprits of gradual injury development due to subtle movement inefficiencies. One such movement is the “hinge at the waist” pattern commonly used when picking up objects from the floor. Without proper hip hinge mechanics, the lumbar spine rounds excessively under load, increasing intradiscal pressure by up to 180% compared to a neutral spine, according to biomechanical studies from the *Journal of Biomechanics*. Over time, this repeated overload contributes to disc herniation and degenerative disc disease.
Another high-risk pattern is the “valgus collapse” during single-leg movements like stepping off a curb or climbing stairs. This collapse-characterized by inward knee movement and inward foot rotation-disrupts the kinetic chain, placing excessive strain on the ACL and medial collateral ligament. Research from the *American Journal of Sports Medicine* found that individuals who demonstrate valgus collapse during landing tasks have a 4.5 times higher risk of ACL injury. Weakness in the gluteus medius and poor ankle dorsiflexion mobility are primary drivers of this dysfunction, both of which can be corrected through targeted mobility exercises.
Even simple seated transitions, such as rising from a chair without using armrests, reveal underlying mobility deficits. A study published in *Gait & Posture* showed that adults over 60 who required arm assistance to stand had 30% lower quadriceps strength and 25% reduced ankle dorsiflexion compared to those who could perform the movement independently. This loss of functional strength and mobility directly correlates with increased fall risk and loss of physical independence in older adults.

Photo by Liliana Drew on Pexels
Evidence-Based Strategies to Restore Safe Movement Patterns
Reversing movement dysfunction requires a systematic approach that integrates mobility, stability, and neuromuscular re-education. The following five-step protocol is grounded in current research and clinical guidelines from the National Academy of Sports Medicine and the American Physical Therapy Association.
- Step 1: Joint-by-Joint Assessment for Imbalances: Begin with a self-screen using the Functional Movement Screen (FMS) or a simple overhead squat test. Look for asymmetries, excessive forward lean, or inability to maintain a neutral spine. These red flags indicate areas where mobility restrictions or stability deficits are present. For instance, if your arms fall forward during an overhead reach, it suggests limited thoracic spine extension and tight pec minor muscles. Addressing these findings before loading movement patterns prevents compensatory injuries.
- Step 2: Tissue-Specific Mobility Drills for Restricted Joints: Focus on restoring joint play before strengthening. For the ankle, use a knee-to-wall dorsiflexion test; if you can’t touch your knee to the wall with your toes 10 cm away, perform ankle mobilizations with a band or foam roller for 2-3 sets of 10 slow repetitions daily. A 2021 study in *Clinical Biomechanics* found that participants who performed ankle mobilizations for four weeks improved dorsiflexion by 8 degrees and reduced knee valgus during landing by 22%.
- Step 3: Activation of Underactive Stabilizers: After improving joint mobility, activate dormant muscles through isometric holds and controlled movements. For the gluteus medius, practice the “clam shell” exercise with a resistance band around the thighs-3 sets of 12 repetitions per side, holding each rep for 3 seconds. This targets the muscle’s role in controlling pelvic alignment during single-leg tasks. Research in the *Journal of Orthopaedic & Sports Physical Therapy* demonstrates that six weeks of gluteus medius activation training reduces knee valgus excursion by up to 34% during dynamic movements.
- Step 4: Integrate Movement Patterns with Load Management: Progress from isolated drills to compound movements using bodyweight or light resistance. The “hip hinge with dowel” exercise teaches proper hip flexion while maintaining a neutral spine. Stand with a dowel along your spine-contact with head, mid-back, and sacrum. Hinge at the hips, pushing your buttocks back, and lower only as far as you can maintain all three points of contact. Perform 3 sets of 8 repetitions, focusing on slow tempo. This drill reduces lumbar flexion during lifting by 40%, according to a 2023 biomechanical analysis in *Medicine & Science in Sports & Exercise*.
- Step 5: Neuromuscular Re-Education Through Unstable Surfaces: Add instability to challenge balance and coordination. Perform step-ups onto a foam pad or balance pad while maintaining a neutral pelvis and controlled knee alignment. Start with 2 sets of 6 repetitions per leg, progressing to 3 sets of 12. A 2022 study in *Frontiers in Physiology* showed that balance training on unstable surfaces improved postural control by 29% and reduced ankle sprain recurrence by 37% in recreational athletes over 12 weeks.
Cutting-Edge Research and Clinical Recommendations
Recent advances in movement science highlight the importance of individualized mobility programming based on tissue-specific needs rather than generalized routines. A 2023 randomized controlled trial in *BMJ Open Sport & Exercise Medicine* compared two groups of office workers: one performing a standardized stretching routine and the other following a customized mobility program based on FMS screening. After 12 weeks, the customized group showed a 58% reduction in reported musculoskeletal pain during work tasks and a 42% improvement in functional movement scores, while the stretching-only group saw no significant change. These findings underscore the limitations of one-size-fits-all approaches in injury prevention.
- Key Finding: A 2023 study in *Sports Health* found that individuals with chronic neck pain who performed cervical spine mobility drills (chin tucks and lateral flexion) for 6 weeks reduced pain intensity by 47% and improved cervical range of motion by 31%, compared to a control group receiving only general advice.
- Expert Consensus: The American Academy of Orthopaedic Surgeons recommends integrating functional mobility exercises into daily routines, especially for individuals with sedentary occupations. Their 2023 position statement emphasizes that “regular mobility drills targeting restricted joints and underactive stabilizers can reduce injury risk by up to 40% in high-risk populations.”
- Future Directions: Emerging research is exploring the use of wearable sensors and AI-driven movement analysis to provide real-time feedback during mobility exercises. Early trials using inertial measurement units (IMUs) have shown a 62% improvement in movement quality adherence compared to traditional coaching methods, suggesting a transformative role for technology in personalized mobility training.
Frequently Asked Questions
How long does it take to see improvements in functional mobility?
While acute changes in joint range of motion can be felt within 2-3 weeks of consistent daily practice, meaningful neuromuscular adaptations require 6-8 weeks. A 2022 study in *Physical Therapy & Rehabilitation Journal* found that participants practicing mobility drills for 10 minutes daily for eight weeks improved their Functional Movement Screen scores by an average of 3.2 points, a clinically significant change associated with reduced injury risk.
Can I do these exercises if I already have chronic pain?
Yes, but under professional guidance. For individuals with persistent pain, especially in the spine or joints, consult a physical therapist before beginning mobility exercises. A 2023 clinical guideline from the Orthopaedic Section of the American Physical Therapy Association recommends starting with pain-free ranges and using isometric holds to activate stabilizers without aggravating symptoms. In one case series, 78% of patients with chronic low back pain reported significant pain reduction after 10 weeks of guided mobility training.
What’s the best time of day to perform functional mobility exercises?
The optimal timing depends on your schedule and goals. Morning sessions are ideal for lubricating stiff joints after sleep, while evening sessions can help release tension accumulated during the day. Research in *Chronobiology International* found that performing mobility drills in the morning improved joint range of motion by 15% throughout the day, while evening sessions reduced perceived stiffness by 22% in sedentary workers.
Are there any exercises that should be avoided if I have poor mobility?
Avoid high-load, high-velocity movements like box jumps or Olympic lifts if you have significant joint restrictions or muscle imbalances. These can reinforce dysfunctional movement patterns and increase injury risk. Instead, focus on controlled, low-velocity mobility drills that emphasize joint centration and neuromuscular control. A 2022 systematic review in *Scandinavian Journal of Medicine & Science in Sports* identified deep squats with excessive forward lean and overhead presses with rib flaring as high-risk movements for individuals with thoracic spine stiffness.
Conclusion and Key Takeaways
Functional mobility exercises are not just another fitness trend-they represent a fundamental shift in how we approach injury prevention and physical independence. By addressing the root causes of movement dysfunction-joint restrictions, muscle imbalances, and neuromuscular inefficiencies-these exercises restore the body’s natural resilience to daily stresses. Whether you’re an athlete, desk worker, or retiree, integrating mobility drills into your routine can transform seemingly ordinary actions into safe, efficient movements.
Start with a joint-by-joint assessment, prioritize tissue-specific mobility, activate dormant stabilizers, and progress gradually into integrated movement patterns. Consistency over time yields measurable improvements in pain reduction, movement quality, and injury resilience. For personalized guidance, consult a qualified movement specialist or physical therapist who can tailor exercises to your unique anatomy and goals. Your body’s ability to move pain-free tomorrow begins with the choices you make today.

